The Link Between ADHD and Eating Disorders: What We Know


- Attention deficit hyperactivity disorder (ADHD) and eating disorders commonly occur together, though they aren’t direct causes of one another.
- Some ADHD traits can make you or a loved one more vulnerable to developing an eating disorder.
- Treatment for an eating disorder when ADHD is present requires a knowledgeable care team who can customize a treatment plan that addresses both conditions.

Attention deficit hyperactivity disorder (ADHD) shows up differently from person to person. But a few common characteristics include difficulty with planning, organizing, focusing, managing time, adjusting to changes or new routines, and more. ADHD is not a character flaw; it’s a neurodevelopmental disorder that presents challenges with executive function, or the way your brain tackles tasks and regulates behaviors. The condition can affect your quality of life or that of a loved one.
In comparison to ADHD, eating disorders are mental health conditions rather than developmental disorders. However, ADHD and eating disorders can significantly overlap. This doesn’t mean that one causes the other, just that they share some characteristics and can occur together.
“ADHD and eating disorders can be intertwined in so many different ways,” says Brittany Lauro, a lead therapist at Equip who also has lived experience with ADHD, “from eating as a way to self-regulate, to forgetting to eat for long periods of time, to feelings of shame or guilt, perfectionism, and body image concerns. ADHD and all different forms of eating disorders can often pair together.”
In this article, we explore ADHD and eating disorders, ADHD eating habits, ADHD and hunger cues, ADHD and appetite, ADHD and overeating, ADHD and impulsive eating, ADHD and food aversion, food noise and ADHD, food hyper-fixation, and more.
Understanding the connection between ADHD and eating disorders
The Venn diagram below shows, in a nutshell, how ADHD and eating disorders overlap through dopamine dysregulation, impulsivity, emotional dysregulation, and more. For those with ADHD, food can be both a stimulant and a tool for coping.
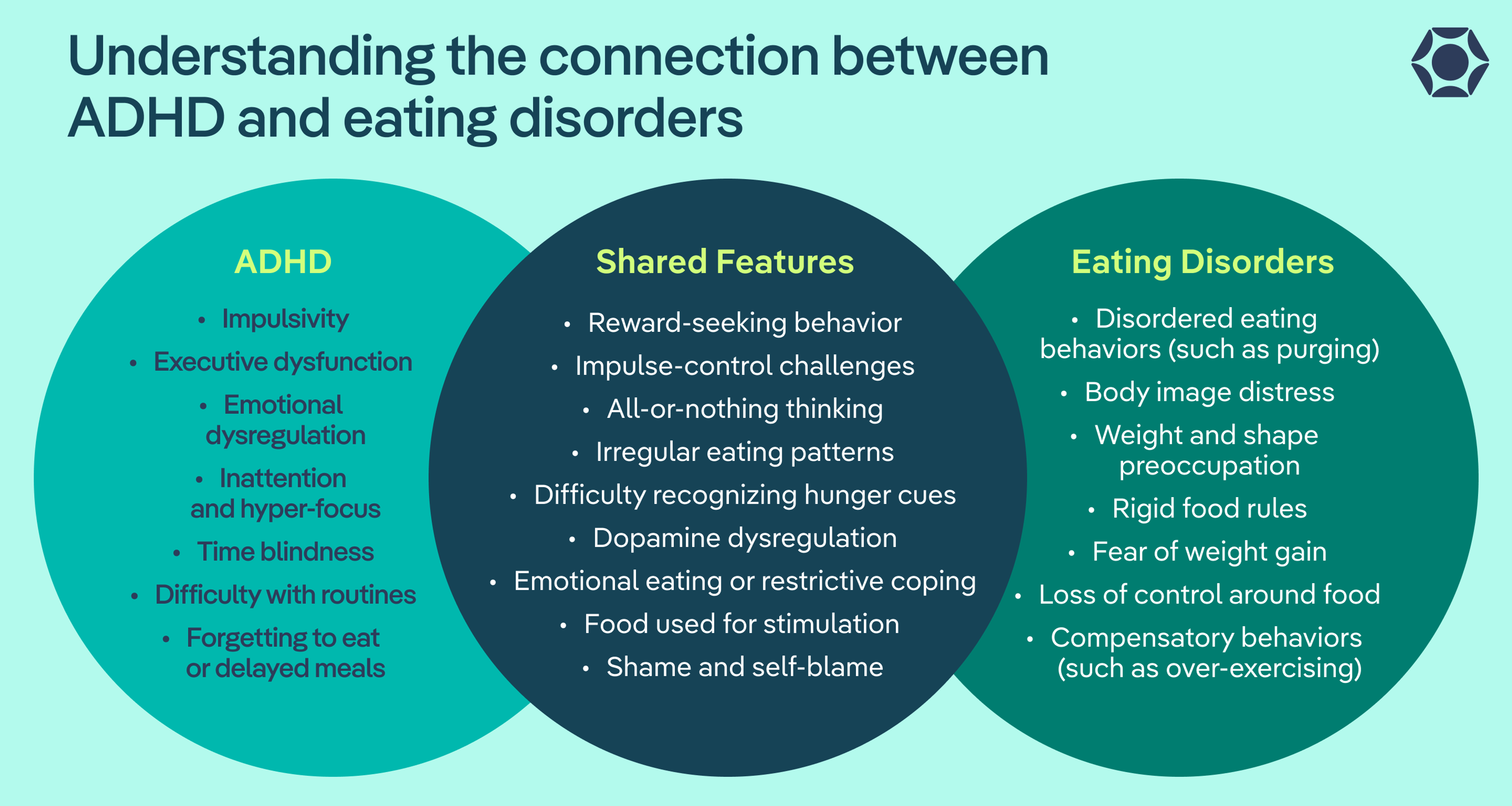
First, let’s unpack what ADHD and eating disorders are, and then we can explore more in depth how their characteristics overlap.
What is ADHD?
ADHD is a neurodevelopmental condition rooted in executive dysfunction. Executive functions are cognitive abilities that help you achieve goals, manage everyday life tasks, adapt to situations, and manage social interactions.
Think of executive functioning as a project manager or coach in your brain. Having executive dysfunction means that your brain’s project manager just operates a little differently than that of the general population’s. Why? The exact cause is uncertain, but it’s potentially due to some structural or functional differences. Regardless of why it happens, executive dysfunction doesn’t mean a person is flawed.
ADHD can affect quality of life, because of having to adjust to a world that often demands high executive functioning. (“In my opinion, the hardest part is living in a society that is designed around a completely different brain type and having to try to get by,” says Lauro). However, the condition is also linked to enhanced creativity, curiosity, adventurousness, determination, resilience, and even energy.
The condition is common. More than 11% of children in the United States have an ADHD diagnosis, while about 6% of adults do. More males tend to get diagnosed than females, especially in childhood or adolescence, but ADHD is underdiagnosed in females because the condition can look a bit different based on sex assigned at birth.
What are eating disorders?
Eating disorders are a group of mental health conditions characterized by disturbances in eating behaviors and, often, a preoccupation with body size or weight. These disturbances can dramatically impact physical, psychological, and social health and overall functioning.
Prevalence varies based on the specific eating disorder. Otherwise specified feeding and eating disorder (OSFED) the most common for females, while pica and rumination disorder are the least common. Binge eating disorder (BED) is the most common for males, while anorexia nervosa (AN) is the least common.
About 14% of males and 20% of females in the United States will experience an eating disorder in their lifetime. However, eating disorders tend to be underdiagnosed in males. This likely stems from the way society tends to assume that eating disorders are largely a female issue, which is a myth. Additionally, stigma plays a role.
How ADHD traits can affect eating patterns
Having ADHD does not cause an eating disorder, and vice versa. But research has long found associations between ADHD and eating disorders. For example, some studies show that 20% of children with ADHD also develop eating disorders.
This means that if you (or a loved one) has ADHD, then you may be more vulnerable to an eating disorder. Likewise, if you have an eating disorder, you might have undiagnosed ADHD.
Some of the commonalities between ADHD and eating disorders can be found in the factors that contribute to both conditions.
A common misconception about eating disorders is that they are caused by a desire to be thin or that they’re rooted in vanity. In reality, eating disorders are complex mental health conditions driven by a variety of factors, including:
- Brain chemistry (including levels of chemical messengers, such as dopamine or serotonin)
- Brain functionality (differences in brain networks and how they work together)
- Childhood trauma or trauma in general
- Cultural norms surrounding body size
- Genetics
- Personality traits such as perfectionism, obsessive-compulsive tendencies, and others
Some of these issues—like genetic and environmental factors and differences in brain chemistry and functionality—can also contribute to ADHD.
Additionally, ADHD traits can affect eating patterns, causing an additional level of vulnerability to developing an eating disorder.
ADHD traits and how they may impact eating behavior
ADHD trait | How the trait shows up | Potential impact on eating behavior |
Dopamine dysregulation | Brain seeks stimulation and reward | Eating (especially highly palatable foods) used for stimulation, comfort, or focus |
Impulsivity | Acting before thinking; difficulty pausing | Eating rapidly, difficulty stopping once started, loss of control around food |
Emotional dysregulation | Intense emotions; difficulty self-soothing | Eating or restricting in response to stress, shame, boredom, or overwhelm |
Executive dysfunction | Difficulty planning, organizing, and initiating tasks | Irregular meals, skipped meals, inconsistent food availability, chaotic eating patterns |
Time blindness | Difficulty sensing passage of time | Long gaps without eating followed by extreme hunger or overeating |
Inattention | Difficulty noticing internal or external cues | Missing hunger or fullness signals; eating mechanically or mindlessly |
Hyper-focus | Intense fixation on a single topic or behavior | Rigid food rules, obsessive tracking, or prolonged restriction without awareness |
All-or-nothing thinking | Difficulty with moderation | Cycles of strict control followed by overeating or abandonment of routines |
Difficulty with routines | Struggle maintaining consistent habits | Unpredictable eating schedules and disrupted appetite regulation |
Sensory sensitivity | Heightened response to taste, texture, smell | Strong food aversions, limited food variety, or reliance on “safe” foods |
Low interoceptive awareness | Difficulty interpreting body signals | Confusion about hunger, fullness, or satiety; eating based on external rules |
Shame sensitivity/rejection sensitivity | Heightened response to perceived failure or judgment | Secretive eating, avoidance of eating with others, rigid self-criticism |
Cognitive overload | Mental fatigue from constant decision-making | Defaulting to convenience foods or alternating between restriction and overeating |
Lauro weighs in on some of the ways ADHD traits and eating disorder traits overlap. “ADHDers may lack internal sensing abilities that neurotypical people have, and thus it may not be realistic for us to rely on our hunger and fullness cues alone,” she says.
Additionally, hunger cues may be absent to a certain extent, since some ADHD medications can suppress appetite while also revving metabolism, leading to weight loss.
“ADHDers are also often sensory seekers,” she says. “Movement helps me focus and regulate. I can think and perform so much better with movement, including ‘sedentary movement.’ Oftentimes, that looks like a lot of snacking on crunchy food items.” She explains that since society somewhat stigmatizes snacking, this can foster feelings of shame or guilt, which may trigger binge eating.
Lauro adds that in order to function, ADHD brains crave dopamine, a neurotransmitter linked to reward, motivation, and pleasure. “There might be a very real and helpful purpose for your desire for highly palatable foods like desserts, chips, etc.,” she explains.
All-or-nothing thinking is also common with ADHD, and this mindset can foster perfectionism. “The thought ‘I will only do this thing if I can perfect it’ or ‘I can only start this task under the right circumstances’ lends itself to perfectionism. There’s a loss of the middle ‘gray’ area,” Lauro says.
“On the one hand,” she adds, “this style of thinking can be great for making decisions in crisis situations. When an eating disorder is in the picture, it can co-opt ADHD and take advantage of the thinking style to use for self-deprivation.”
For example, if you’ve eaten something that you’ve deemed “off-limits,” a donut for example, then you might decide you cannot eat anything for the rest of the day because of having consumed this “bad” food.
She also notes that ADHD can lead to feeling as if you need to hide or mask parts of yourself. “This can play into perfectionism and fuel the belief that one must look, dress, or act a certain way in order to fit in and be accepted,” she explains. Again, society tends to expect everyone to have the same types of executive function. But with ADHD, your executive function simply looks different. This may drive you to hide your ADHD or to “fit in” in other ways you might perceive as a societal expectation, such as by being as thin as possible.
“Time blindness” is another common ADHD trait. This can refer to a few things, like getting overly focused on something and not realizing that time has gone by, or having difficulty estimating how long a task will take.
“Hyper-focus is a tricky situation,” Lauro says. “Most commonly we see this dance with eating disorders as a means of restriction. ADHD can make it hard to remember to eat, especially when you’re ‘locked in’ on a task in front of you.” She adds that an “eating disorder loves to take advantage of this to support the restriction part of the eating disorder cycle.”

Lauro is quick to point out that traits related to ADHD that can make someone more vulnerable to an eating disorder can also be beneficial for eating disorder recovery. These traits can include perfectionism or hyper-focus, both of which have benefits as well as drawbacks.
“It’s really easy to have these conversations from a neurotypical lens,” she says, “but that often positions neurotypical brains as superior, and I respectfully disagree with that notion. I’ve seen so many instances where those traits are the exact features that let someone with ADHD ‘lock in’ to applying all of the evidence-based interventions and achieving recovery.”
ADHD and specific eating disorders
The connections between ADHD and eating disorders differ depending on the specific eating disorder. So let’s take a brief look at how certain traits might match up to different eating disorder diagnoses.
Eating Disorder Context | ADHD Traits Most Involved | How ADHD Traits May Apply to Eating Behaviors |
ADHD & binge eating disorder | Impulsivity, dopamine dysregulation, emotional dysregulation, executive dysfunction | Food used for stimulation or dopamine-seeking; difficulty stopping once eating begins; binge episodes triggered by emotional overwhelm or extreme hunger after missed meals; reduced pause between urge and action |
ADHD & avoidant/ restrictive food intake disorder (ARFID) | Sensory sensitivity, inattention to hunger cues, executive dysfunction, rigidity, hyper-focus | Avoidance driven by texture, taste, smell, or appearance; limited food variety; difficulty planning or preparing acceptable foods; inconsistent intake due to reduced perception of hunger and satiety cues, rather than body weight or shape concerns |
ADHD & bulimia nervosa | Impulsivity, emotional dysregulation, all-or-nothing thinking, shame sensitivity | Cycles of loss of control followed by compensatory behaviors; rapid escalation from urge to action; heightened guilt and secrecy; difficulty interrupting binge-purge patterns once initiated |
ADHD & anorexia nervosa | Hyper-focus, need for structure, cognitive rigidity, reward sensitivity | Restriction reinforced by hyper-focus on rules, numbers, or control; rigid routines provide external structure; difficulty shifting away from entrenched behaviors; restriction may temporarily improve focus or reduce internal chaos |
Why ADHD and eating disorders are often missed or misunderstood
Both ADHD and eating disorders often go undiagnosed, and Lauro says this is because they are misunderstood disorders.
“It’s true that not many providers, across various fields, receive training on ADHD or eating disorders,” she says. “ADHD and eating disorders often get overlooked, being chalked up to a person ‘just being lazy’ or unmotivated.” And weight loss can get lauded as a good “lifestyle change” when it may be the manifestation of an eating disorder.
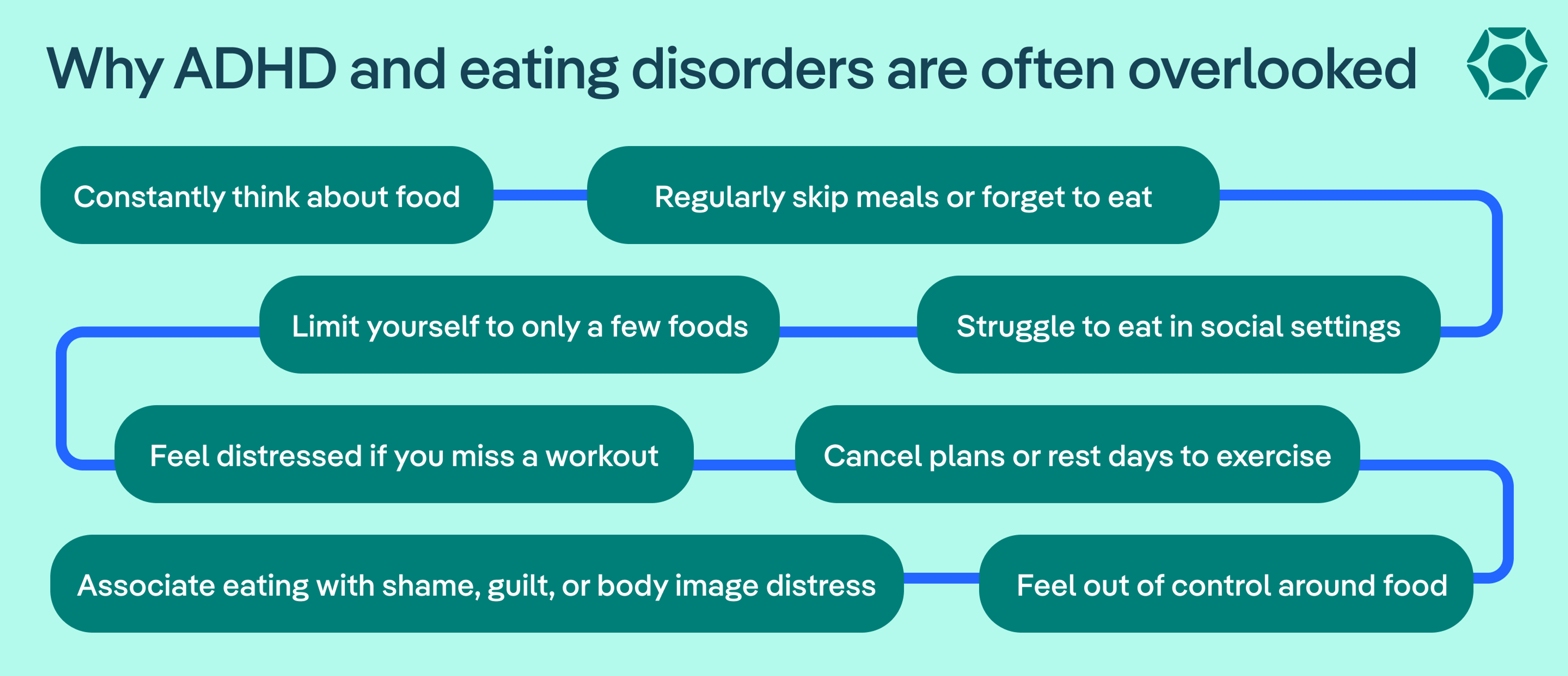
She recommends seeking help if you (or a loved one):
- Think about food for the majority of your day, sometimes referred to as “food noise”
- Go for long periods without eating, whether intentionally or accidentally forgetting to eat
- Experience distress when not working out or when you can’t fit exercise in
- Skip other plans or rest days to work out
- Feel out of control with food
- Have only a few specific foods that you eat, whether from aversion or food restriction
- Link eating to shame, guilt, or body image distress
- Face difficulty eating in social situations
What treatment looks like when someone has ADHD and an eating disorder
If you or a loved one has ADHD and an eating disorder or a suspected one, treatment is within reach. A common perception is that people with ADHD will have difficulty with treatment, but that’s false.
“Oftentimes ADHDers are the ones who excel in evidence-based care,” Lauro says, “particularly the structured evidence-based care models.”
Treatment requires looking at the process through an ADHD lens, however. Lauro shares a few examples.
“This could look like flexibility or digital accommodations for completion of tasks like self-monitoring tools and monitoring records,” she says. “It could also include discussions of how to plan-in certain meals or snacks to help with regulation and focus.”
She adds, “We also often talk about establishing a regular pattern of eating—and maintaining this goal over relying only on intuitive eating.”
Sometimes treatment requires modifications based on sensory needs. “Many ADHDers might be ‘super sensors,’” Lauro explains, “and one way we can improve eating is by addressing areas of overstimulation, like sound, by incorporating ear plugs.” That’s just one example, however.
At Equip, eating disorder recovery occurs through a team-based approach that’s individualized to you (or your loved one). This means that if ADHD is a factor, clinicians and other providers will work to understand the specific ADHD traits that are present and how they may be affecting eating, exercise, or purging patterns. The team will also tailor treatment to your unique needs, or those of a loved one.
The bottom line
ADHD and eating disorders share some strong connections, including what drives them, behaviors and traits associated with them, and more. If you have ADHD, you might be more vulnerable to developing an eating disorder. And if you have an eating disorder, you might also have ADHD. But they don’t always occur together. The associations are just something to be aware of.
The good news is that ADHD traits can also be an asset for eating disorder recovery. The bottom line is that help is available, and knowledgeable clinicians can tailor eating disorder recovery to you and your unique needs.
FAQ
Does ADHD affect eating habits?
Yes, ADHD can affect eating habits in multiple ways, including leading to forgetting to eat because of missed hunger cues, binge eating for dopamine release or emotional regulation, and more. Having ADHD can make you more vulnerable to developing an eating disorder because of these issues.
Can ADHD cause food aversion?
Yes, if you have ADHD, you might have sensory concerns regarding certain food textures, smells, appearances, tastes, or even how foods sound when you eat them. You might also have reduced appetite from ADHD medications or reduced hunger cues in general.
How do you treat ADHD and an eating disorder together?
Treating an eating disorder when ADHD is present requires considering the specific traits unique to your experience with ADHD and how those traits might contribute to the eating disorder you have. Additionally, eating disorder treatment should be tailored to the ways in which you best learn or adapt to situations.
Appolinario, Jose Carlos, et al. “Associations of Adult ADHD Symptoms with Binge Eating Spectrum Conditions, Psychiatric and Somatic Comorbidity, and Healthcare Utilization.” Revista Brasileira De Psiquiatria (Sao Paulo, Brazil: 1999), vol. 46, 2024, p. e20243728.
Babinski, Dara E. “Sex Differences in ADHD: Review and Priorities for Future Research.” Current Psychiatry Reports, vol. 26, no. 4, Apr. 2024, pp. 151–56.
Balasundaram, Palanikumar, and Prathipa Santhanam. “Eating Disorders.” StatPearls, StatPearls Publishing, 2025.
CDC. “Data and Statistics on ADHD.” Attention-Deficit / Hyperactivity Disorder (ADHD), 19 Nov. 2024.
Cristofori, Irene, et al. “Executive Functions.” Handbook of Clinical Neurology, vol. 163, 2019, pp. 197–219.
Dalnoki, Laura, et al. “Exploring the Relationship of Dietary Intake with Inattention, Hyperactivity, and Impulsivity, Beyond ADHD.” Journal of Attention Disorders, vol. 29, no. 1, Jan. 2025, pp. 70–79.
Esperón, CA Soutullo, and T. T. Babatope. “Attention Deficit Hyperactivity Disorder and Eating Disorders: An Overlooked Comorbidity?” Anales Del Sistema Sanitario de Navarra, vol. 45, no. 1, Apr. 2022, p. e0994.
Kaşak, Meryem, et al. “Selective Eating and Sensory Sensitivity in Children With ADHD: A Comparative Study of ARFID Symptom Profiles.” The International Journal of Eating Disorders, vol. 58, no. 10, Oct. 2025, pp. 1991–2002.
Magnus, Warren, et al. “Attention Deficit Hyperactivity Disorder.” StatPearls, StatPearls Publishing, 2025.
Martin, Elizabeth, et al. “Interoceptive Accuracy Mediates the Longitudinal Relationship between Attention Deficit Hyperactivity Disorder (ADHD) Inattentive Symptoms and Disordered Eating in a Community Sample.” Physiology & Behavior, vol. 268, Sept. 2023, p. 114220.
Mette, Christian. “Time Perception in Adult ADHD: Findings from a Decade-A Review.” International Journal of Environmental Research and Public Health, vol. 20, no. 4, Feb. 2023, p. 3098.
Nordby, Emilie S., et al. “Silver Linings of ADHD: A Thematic Analysis of Adults’ Positive Experiences with Living with ADHD.” BMJ Open, vol. 13, no. 10, Oct. 2023, p. e072052.
Pan, Mei-Rong, et al. “Bidirectional Associations between Maladaptive Cognitions and Emotional Symptoms, and Their Mediating Role on the Quality of Life in Adults with ADHD: A Mediation Model.” Frontiers in Psychiatry, vol. 14, July 2023, p. 1200522.
Ravi, Prithvi, and Safeera Khan. “Attention Deficit Hyperactivity Disorder: Association with Obesity and Eating Disorders.” Cureus, vol. 12, no. 12, Dec. 2020, p. e12085.
Staley, Brooke S. “Attention-Deficit/Hyperactivity Disorder Diagnosis, Treatment, and Telehealth Use in Adults — National Center for Health Statistics Rapid Surveys System, United States, October–November 2023.” MMWR. Morbidity and Mortality Weekly Report, vol. 73, 2024.
Villa, F. M., et al. “ADHD and Eating Disorders in Childhood and Adolescence: An Updated Minireview.” Journal of Affective Disorders, vol. 321, Jan. 2023, pp. 265–71.
Ward, Zachary J., et al. “Estimation of Eating Disorders Prevalence by Age and Associations with Mortality in a Simulated Nationally Representative US Cohort.” JAMA Network Open, vol. 2, no. 10, Oct. 2019, p. e1912925.
Yao, Shuyang, et al. “Associations Between Attention-Deficit/Hyperactivity Disorder and Various Eating Disorders: A Swedish Nationwide Population Study Using Multiple Genetically Informative Approaches.” Biological Psychiatry, vol. 86, no. 8, Oct. 2019, p. 577.
Yasui‐Furukori, Norio. “Editorial: Deciphering Dopamine Dysregulation in Adult ADHD.” PCN Reports: Psychiatry and Clinical Neurosciences, vol. 4, no. 3, June 2025, p. e70151.







