What Are the Different Levels of Care for Eating Disorders?


- When considering treatment, you’ll need to make a decision about the needed level of care for yourself or a loved one.
- Gaining clarity on your options will help you understand what’s best for your recovery.
- Levels of care range from outpatient (including virtual) options to full-time residential care or even hospitalization if necessary.
- Treatment is available and recovery is possible with the help of a knowledgeable care team.

If you’re wading through eating disorder treatment options for yourself or a loved one and have become overwhelmed with all the different types, you’re not alone. What’s an IOP and what’s a PHP? Where does virtual care fit in and how does it work? These might be some of the questions racing through your mind.
Take a deep breath and exhale. The two key things to know right away is that care is available and that you do have options when considering the type that’s best for you or a family member.
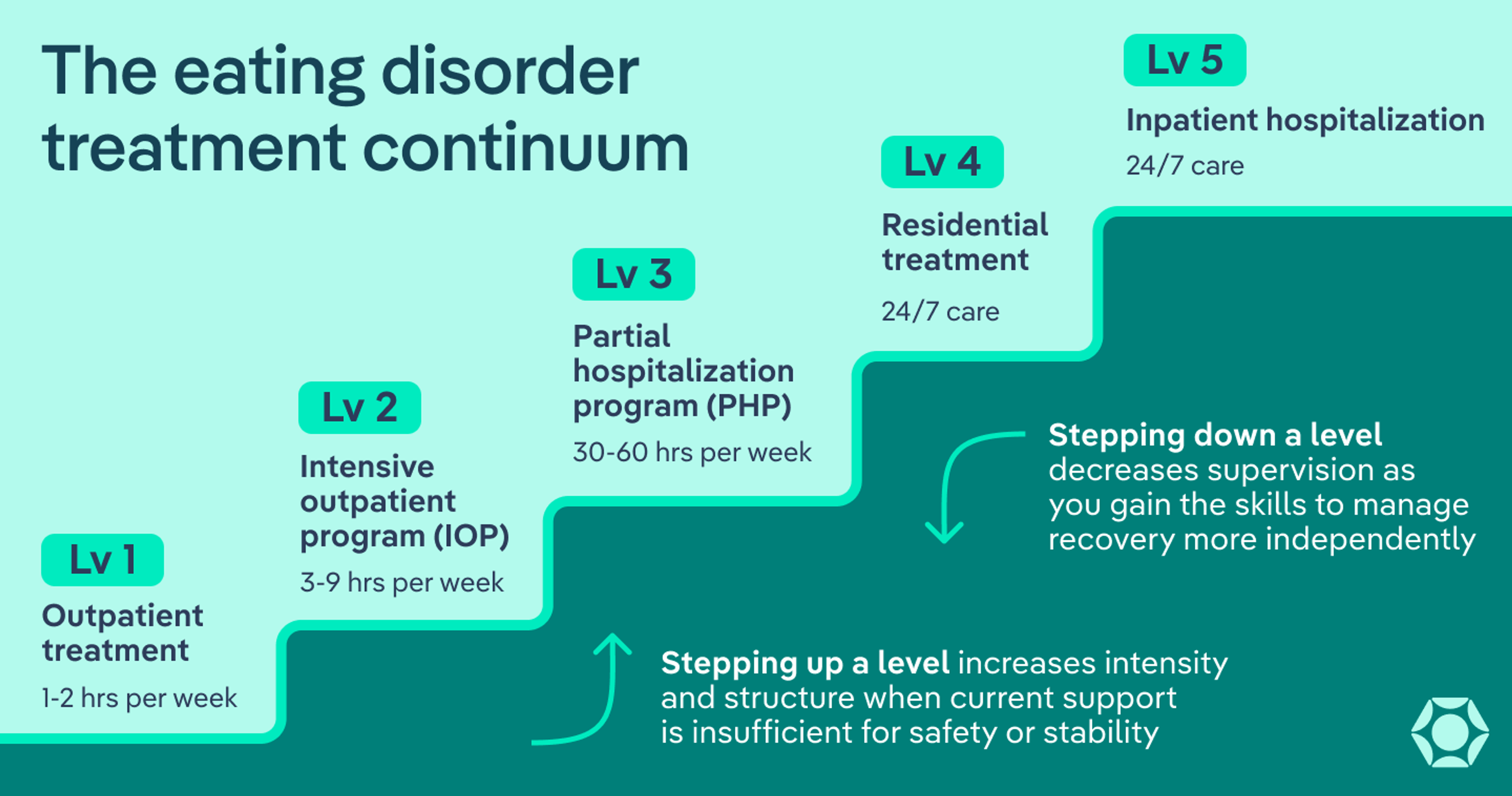
To unpack it all, think of levels of care for eating disorders as a continuum. The spectrum ranges from care on an outpatient basis (once a week or more) to around-the-clock care with inpatient hospitalization (which usually lasts for a few days or weeks).
Ultimately, eating disorder care is not one-size-fits all. What’s right for your circumstances may not be right for someone else. People often progress between levels of care as circumstances or needs change.
In this article, we explore the different levels of care for eating disorders and how they operate. We’ll help you determine what level of care is right for you or your loved one based on individual factors.
What are the levels of care for eating disorders?
The levels of eating disorder care include outpatient options (virtual and/or in person), an intensive outpatient program (IOP), a partial hospitalization program (PHP), residential treatment, and inpatient hospitalization.
Think of these levels of care as existing on a continuum rather than as strict categories. You might even picture a staircase where you can either “step up” or “step down” in care as needed.
“Eating disorder treatment should be tailored to meet patient and family needs,” says Barbara Kessel, DO, CEDS, the supervising psychiatrist at Equip Health.
“Now, that doesn’t mean just anything will work,” she adds. “It is important that people seek treatment rooted in evidence-based practices. But we also know eating disorder recovery will not work if it does not fit into someone’s life. This means that treatment can vary from person to person.”
Outpatient treatment
- Time commitment
- Per week: 1 to 2 hours
- Duration: As long as needed
- Virtual option: Yes
- Living situation: At home, attending weekly sessions
- Level of structure: Minimal and flexible
- Best for: Patients who are medically stable and need flexibility
Outpatient treatment for eating disorders is best for patients who are medically stable. This means you or your loved one is not currently at risk for malnutrition or serious physical or mental health complications.
Outpatient treatment options typically include one-on-one sessions with a mental health professional. And you or a loved one might have occasional additional sessions with a registered dietitian and a medical provider.
Treatment may occur in person or virtually through video conferencing or other methods.
Intensive outpatient program (IOP)
- Time commitment
- Per week: 3 to 9 hours
- Duration: 3 months to 1 year
- Virtual option: Yes
- Living situation: At home, attending various sessions throughout the week
- Level of structure: More structured than regular outpatient treatment but still flexible
- Best for: Patients who need a higher level of care than can be provided with weekly sessions but who need flexibility
You or your loved one might need a more intensive and structured form of outpatient care. An IOP includes the same elements as a regular outpatient program. But rather than solely meeting with individual providers, you’ll experience more of a coordinated care approach. This type of care integrates other elements such as meals and/or support groups.
IOPs can be built around attending school or going to work. And they can be done virtually or in person.
Partial hospitalization program (PHP)
- Time commitment
- Per week: 30 to 60 hours
- Duration: several weeks to several months
- Virtual option: Yes
- Living situation: At home, attending sessions on most days
- Level of structure: Highly structured
- Best for: Patients who need more extensive care than what can be achieved with regular outpatient or IOP care but who are stabilized enough to live at home
The term “partial hospitalization program” for eating disorders can be a bit misleading because it doesn’t involve overnight stays, and the program typically doesn’t take place in a hospital. Instead, care might be received in another type of in-person setting or even virtually.
PHPs for eating disorders are day programs. You or a loved one will spend about six to 10 hours a day receiving care on five to six days per week. Care typically includes individual and group therapy, meal support, and more.
You can complete a PHP in person or virtually. However, because of the time commitment, you or a loved one won’t be able to attend school or work.
Residential treatment
- Time commitment
- Per week: 24/7
- Duration: a few weeks to a few months
- Virtual option: No
- Living situation: On site
- Level of structure: Fully structured
- Best for: Patients who need around-the-clock care and monitoring but who are medically stable
Live-in treatment ranges from residential care for eating disorders to inpatient hospitalization. A live-in setting might be right for you or a loved one if an outpatient program or PHP doesn’t provide enough structure. This might be the case if eating disorder behaviors, such as restriction, bingeing, compulsive exercise, etc., are still present and affecting everyday life.
Residential treatment for eating disorders requires ongoing overnight stays in a treatment center or a smaller facility such as a group home. There, you or a loved one will receive ongoing care, including meals, individual and group therapy, and more.
Working during a residential stay isn’t possible. However, some online learning may be feasible.
Inpatient hospitalization
- Time commitment
- Per week: 24/7
- Duration: a few days to weeks or months
- Virtual option: No
- Living situation: On site
- Level of structure: Fully structured
- Best for: Patients who meet eating disorder hospitalization criteria because of their need for medical stabilization, psychiatric care, or both—around the clock.
Inpatient hospitalization occurs in a hospital setting to offer close care and support for you or a loved one. It may involve:
- Medical stabilization: Eating disorders can lead to severe health concerns, such as complications from malnutrition or purging. Medical stabilization, including renourishment, may be necessary as a first course of action in eating disorder recovery.
- Inpatient psychiatric care: Eating disorders are associated with psychiatric risks, including self-harm. Ongoing psychiatric care and monitoring may be necessary as a safety precaution.
- Inpatient eating disorder medical-psychiatric hospitalization: Some hospital systems have specialized units where you or a loved one can receive both medical stabilization and psychiatric care.
How each level of care compares
The following table shows how the levels of care stack up, starting with the least structured and least time-intensive to the most structured.
Level of care | Time commitment | Typical duration | Virtual option | Living situation | Level of structure | Best for |
Outpatient Treatment | 1-2 hours per week | As long as needed | Yes | Living at home; attending weekly sessions | Minimal and flexible | Patients who are medically stable and need flexibility |
Intensive Outpatient Program (IOP) | 3-9 hours per week | 3 months to 1 year | Yes | Living at home; attending multiple sessions during the week | Moderately structured but still flexible | Patients who need more support than weekly therapy but still require flexibility for work or school |
Partial Hospitalization Program (PHP) | 30-60 hours per week (about 6-10 hours per day, 5-6 days per week) | Several weeks to several months | Yes | Living at home; attending a day program most days | Highly structured | Patients needing more intensive care than IOP but stable enough to live at home |
Residential Treatment | 24/7 care | A few weeks to a few months | No | Living on site at a treatment facility | Fully structured with ongoing supervision | Patients needing constant support and monitoring but who are medically stable |
Inpatient Hospitalization | 24/7 care | A few days to weeks or months | No | Living in a hospital setting | Fully structured with medical supervision | Patients requiring medical stabilization, psychiatric care, or both |
How do you know what level of care you or your loved one may need?
You don’t have to make the decision alone on the type of care needed for you or a loved one. Instead, a medical or mental health clinician can help you decide or guide you in the right direction.
“Recommendations will depend on several factors,” says Dr. Kessel, “such as the severity of your illness; your level of support; your geographic location; your ability to take time away from work, school or family; and what your insurance covers.”
Eating disorder care has also come a long way in the past few decades, offering more flexibility.
“Previously, people seeking comprehensive eating disorder treatment with a unified team had to go to residential facilities or partial hospitalization programs,” Dr. Kessel says. “Now, thanks to innovation and the advent of telehealth services, people can get quality eating disorder treatment wherever they have an internet connection.”
Virtual care will not be right for everyone, depending on factors, such as medical stability, family structure, and co-occurring conditions. But it could be part of a long-term care plan after medical or psychiatric stabilization.
What does it mean to “step up” or “step down” in care?
You aren’t locked into a specific level of care. You can expect to progress in your level of care as needed while you move toward recovery. Think of outpatient care as the most stepped-down option. Higher levels of care (HLOC treatment), include IOPs, PHPs, residential, and inpatient hospitalization.
“People can move between levels of care depending on their individual needs,” Dr. Kessel adds. “While stepping up to medical stabilization or residential care can help a recovery journey—for the most part, we want people to get better in the least restrictive treatment environment that works for them.”
Where does virtual treatment fit into levels of care?
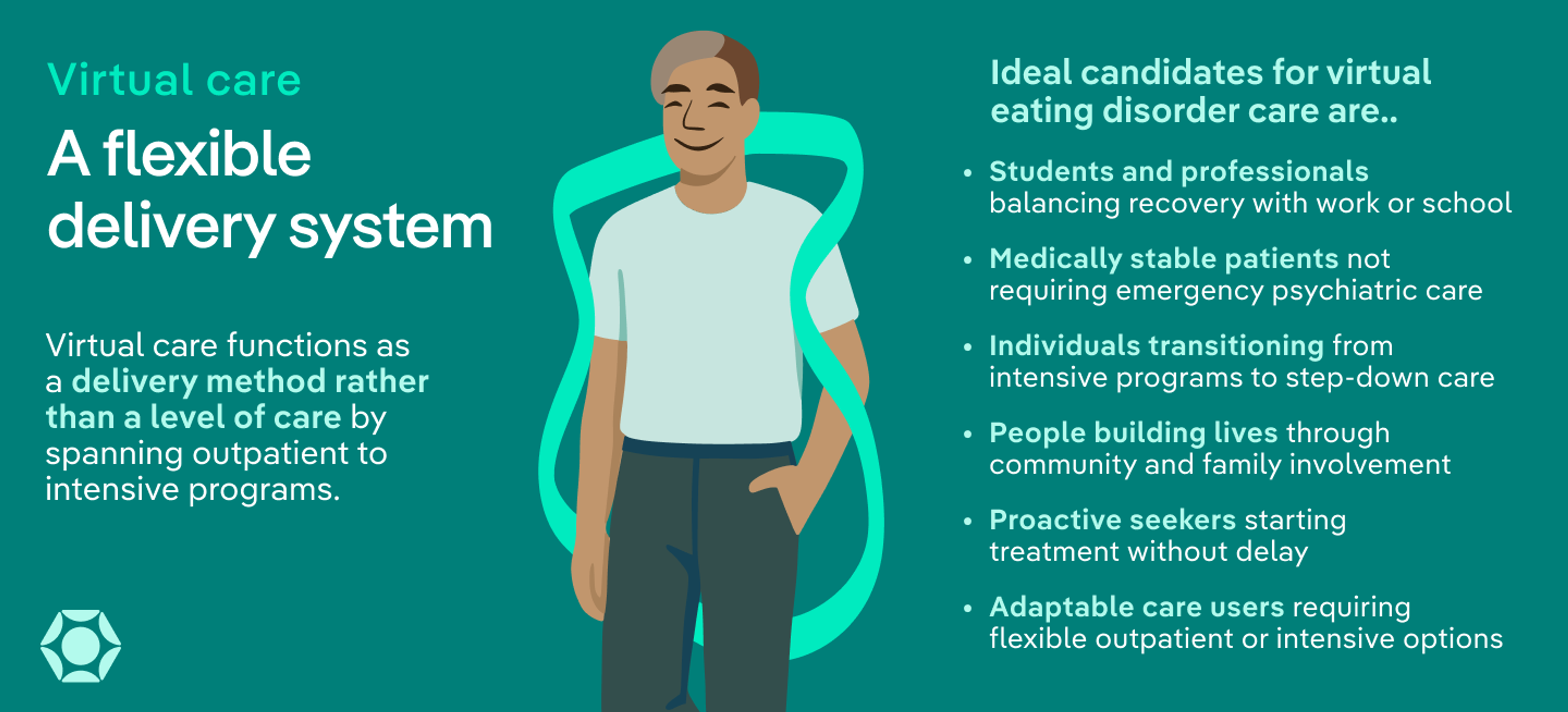
Virtual eating disorder treatment is not a level of care. Instead, it is a delivery system. Virtual care offers flexibility and can be beneficial for receiving eating disorder treatment alongside attending school or work. It can be part of a HILOC option or stepped-down care.
Virtual care serves as an option if eating disorder behaviors are present but you or a loved one is medically stable and not experiencing psychiatric concerns that warrant a HILOC.
For example, “Equip allows people to continue working, attending school, and participating in their families and communities alongside comprehensive, evidence-based eating disorder treatment,” Dr. Kessel explains. “This can provide the flexibility people need to get treatment now, rather than waiting until ‘the right time’ or until they have no other choice.”
Equip is an appropriate level of care for all medically stable patients and an appropriate alternative for patients who might otherwise consider residential, PHP, IOP, or outpatient. Not all virtual care is the same. Some virtual care involves individual sessions only. You can also find virtual IOPs and PHPs. Equip is adaptable, and your level of care changes as you move through recovery.
In other cases, virtual options come into play after a step down in care. “Things in the real world are very different than in treatment centers,” she adds. “And most people need ongoing support when leaving a treatment center or hospitalization.”
Virtual care, in these cases, allows you or a loved one to practice necessary everyday skills under the guidance of a treatment team.
“An important step in recovery is building a life worth living outside of the eating disorder,” Dr. Kessel says. “This means building real-life relationships, having passions to follow and giving your life purpose—all things done outside of treatment sessions.”
Where do different treatment approaches fit in?
You might be wondering how different treatment approaches fit into the different levels of care. Different treatment approaches can generally be used at any level of care. The table below defines some of the most common eating disorder treatment modalities, as well as the settings in which they're commonly used.
Treatment | Definition | Levels of care |
Family-based treatment (FBT) | A therapy approach in which parents or caregivers have an active role in helping a person restore weight and normalize eating behaviors | Outpatient, IOP, PHP; sometimes incorporated into residential programs for adolescents through family sessions |
Cognitive behavioral therapy (CBT) | A structured psychotherapy that focuses on identifying and changing unhelpful thoughts, beliefs, and behaviors that contribute to an eating disorder | Outpatient, IOP, PHP, residential; sometimes adapted during inpatient stabilization |
Dialectical behavior therapy (DBT) | A therapy that combines CBT with mindfulness and emotional regulation skills | Outpatient, IOP, PHP, residential, and inpatient programs where structured skills training groups are common |
Temperament-based therapy with support (TBT-S) | A therapy that focuses on temperament’s role in eating disorders and involves parents or caregivers as active supports. | Outpatient, IOP, PHP, and residential settings |
Exposure and response prevention (ERP) | A behavioral therapy that gradually exposes you or a loved one to triggers while helping to change coping mechanisms. | Outpatient, IOP, PHP, and residential settings |
Acceptance and commitment therapy (ACT) | A mindfulness-based therapy that encourages you or a loved one to accept difficult thoughts and feelings while committing to behaviors aligned with personal values | Outpatient, IOP, PHP, and residential settings |
Interpersonal psychotherapy (IPT) | A therapy focused on improving interpersonal relationships and resolving social or role conflicts that may contribute to mental health symptoms. | Primarily Outpatient, but sometimes used in IOP or PHP programs. |
What questions should you ask when choosing a treatment program?
As you are considering treatment providers or programs, here are some of questions you may want to ask to help guide your decision:

- What experience do you have with treating eating disorders?
- What credentials or special training do you have related to eating disorders?
- Do you belong to any eating disorder treatment professional organizations, such as the Academy for Eating Disorders (AED) or the International Association of Eating Disorders Professionals (iaedp)?
- How long will treatment last, and what will it cost?
- How do you set treatment priorities and goals?
- How do you measure progress in recovery?
- What is the role of family or other loved ones in treatment?
- What is your readmission rate? (for PHP, residential, and inpatient programs)
- Do you provide the option of virtual sessions?
The bottom line
Finding the right level of care can take time. And that’s OK. Keep in mind that there isn’t one “right” way to get started with eating disorder treatment.
Even after extensive research, you might still go through some trial and error to find the right fit. The recovery process isn’t usually simple or linear. It’s hard work, but it’s worth it. You can schedule a low-pressure, free consultation here to talk through the available treatment options and see whether Equip might be a good fit for your unique needs.
FAQ
What is considered a higher level of care for eating disorders?
Higher levels of care (HILOC) for eating disorders include an intensive outpatient program (IOP), a partial hospitalization program (PHP), residential treatment, and inpatient hospitalization.
What is the difference between residential treatment and inpatient hospitalization?
Residential treatment and inpatient hospitalization sound similar but they are different. Residential treatment involves 24/7 care and monitoring at a residential facility. Residential facilities include large treatment centers or smaller settings, such as group homes. In-patient hospitalization includes 24/7 care and monitoring in a hospital. It is necessary when you or a loved one needs to be medically or psychiatrically stabilized for health and safety reasons.
What is the difference between IOP and PHP for eating disorders?
Although both options allow you or a loved one to live at home, an intensive outpatient program (IOP) is different from a partial hospitalization program (PHP). An IOP involves three to nine hours of care per week, while a PHP involves 30 to 60 hours. Care can occur in person or virtually, depending on individual needs.
Can someone work or go to school while in eating disorder treatment?
In some cases, you can work or go to school while in eating disorder treatment. You or a loved one will have this option with outpatient and intensive outpatient (IOP) care. Remember that virtual options are possible and offer the most flexibility.
Bryant, Emma, et al. “Treating the Individual: Moving towards Personalised Eating Disorder Care.” Journal of Eating Disorders, vol. 13, Apr. 2025, p. 63.
Derenne, Jennifer. “The Role of Higher Levels of Care for Eating Disorders in Youth.” Child and Adolescent Psychiatric Clinics of North America, Eating Disorders in Child and Adolescent Psychiatry, vol. 28, no. 4, Oct. 2019, pp. 573–82.
Novack, Kaylee, and Nicholas Chadi. “The Hybrid Space in Eating Disorder Treatment: Towards a Personalized Approach to Integrating Telehealth and in-Person Care.” Journal of Eating Disorders, vol. 13, Feb. 2025, p. 22.







